It’s time for us to cover some basic information about vitamin A as relates to plant-based diets.
First, I’ll answer some common questions for those of you who are in a rush.
- Is vitamin A vegan? Yes, unlike vitamin D (check out the article here) and vitamin B12, vitamin A is found in numerous plant foods.1 As for supplements, provitamin A (carotenoids) are chemically synthesized and thus considered vegan.45 Retinol is animal-derived and not considered vegan. Whether vitamin A palmitate is vegan depends on how the palmitic acid is sourced. Palmitic acid is a fatty acid that is commonly sourced from palm oil but can be derived from animals.46 To know for sure, you will need to search for manufacturer-specific information regarding the ingredients of a specific product.
- What are some vegan sources of vitamin A? Common vegan sources of vitamin A include sweet potatoes, spinach, carrots, pumpkin, butternut squash, cantaloupe, and persimmons. (See the chart below for more examples).2
- Are vegans commonly deficient in vitamin A? No, not characteristically. According to NIH, those at risk for vitamin A deficiency include individuals with cystic fibrosis, premature infants, pregnant and lactating women in developing countries, and young children in developing countries.2
- Do vegans get too much vitamin A and are they at risk for vitamin A toxicity? No, vitamin A in plant foods isn’t pre-formed. The body only makes the vitamin A that it needs from the carotenoids provided via plant sources. The only side effect from eating high amounts of carotenoids from plant foods is a benign condition known as carotenodermia, wherein the skin takes on an orange appearance.2
What we’ll do next is take a closer look at the plant sources of vitamin A as well as some other basic info.
Overview
Vitamin A (Pre-formed)
Vitamin A (aka pre-formed vitamin A) refers to a group of four structurally similar compounds collectively known as retinoids. These compounds have something important in common in that they all exert the vitamin activity of all-trans-retinol.
The molecules include:
- Retinol
- Retinal aka retinaldehyde
- Retinoic acid
- Retinyl ester
They’re known as pre-formed vitamin A, as the body makes these compounds from precursor molecules found in plant foods, or acquires them pre-formed in animal products.
In case you’re interested in the chemistry, retinoids contain:
- A β-ionone ring
- A polyunsaturated side chain
- An alcohol group (retinol), an aldehyde group (retinal), a carboxylic acid group (retinoic acid), or an ester group (retinyl ester).
The side chain is composed of what is known as isoprenoid units (four to be exact) that have a series of conjugated double bonds that can exist in a cis or trans configuration (the latter as in all-trans-retinol).
Carotenoids: The Vitamin A Precursors
Carotenoids refer to a group of more than 600 fat-soluble orange, yellow, and red plant pigments. Collectively, they’re referred to as provitamin A, as some (<10%) are thought to exhibit vitamin A activity. That is, less than 60 can be used by the body to make retinol.
As for the chemistry, carotenoids are made up of an expanded carbon chain having conjugated double bonds, often with an unsubstituted β-ionone ring at one end. Don’t worry, you don’t need to know that.
Of primary importance are three provitamin A carotenoids (typically in all-trans form but can occur in cis form):
- β-carotene—beta carotene is the famous orange pigment found in sweet potatoes, pumpkins, etc.
- α-carotene
- β-cryptoxanthin
Other carotenoid phytochemicals that are thought to help account for the positive health effects associated with high consumptions of carotenoid-rich fruits and veggies include:
- Lycopene—a β-carotene analog found in tomatoes and watermelons.
- Oxycarotenoids—aka oxygenated carotenoids. These include canthaxanthin, lutein, and zeaxanthin.
Functions
Pre-formed Vitamin A
Initially, vitamin A was found to be an important growth factor (GF) in animal foods.
It’s recognized as being essential for a number of reasons including:
- Vision
- Cellular differentiation, growth, and reproduction
- Immune function
- Bone development
Vision
Phototransduction is the fancy name for the process by which light is converted into electrochemical signals in the brain.
Many biological processes require vitamin A in the form of all-trans retinoic acid or 9-cis retinoic acid. For vision, however, it’s the 11-cis retinal form that’s needed. Namely, it has to bind to the protein opsin of visual pigments to facilitate the phototransduction process.
Gene Expression
There are two forms of vitamin A that are thought to regulate gene expression: all-trans retinoic acid and 9-cis retinoic acid. These two molecules find their way inside of the cells’ nucleus where they bind to specific parts of the DNA exerting effects on how genes are expressed.
Two iLBPs (intracellular lipid-binding proteins) transport retinoic acid into the nucleus where they bind to different nuclear receptors.
One iLBP called CRABP II (cellular retinoic acid–binding protein II), carries the vitamin to RARs (retinoic acid receptors), while the other iLBP (fatty acid–binding protein 5) takes the vitamin to PPAR (peroxisome proliferator-activated receptors) β/δ. All-trans retinoic acid binds/activates various RARs and PPAR β/δ, while 9-cis retinoic acid binds/activates RAR and certain RXR receptors (retinoid X receptors).
Through different processes involving RARE (retinoic acid response elements) in the promoter regions on DNA, vitamin A causes receptors to undergo conformational changes that promote the transcription of certain retinoic acid-regulated genes. The specific genes affected by retinoic acid are largely unknown but are thought to code for enzymes, growth factors, and transcription factors that govern certain processes like cell death, or apoptosis.
Cellular Differentiation
Differentiation is the process in which an immature cell undergoes a transformation into a certain type of mature cell. Vitamin A, as retinoic acid, is required by many cells for this process.
Epithelial Cells (Skin and GI Tract)
Epithelial cells are a good example. They’re found in the skin, respiratory and gastrointestinal tracts. Skin medications for acne such as tretinoin are thought to exert their anti-aging effects for this reason—by promoting cellular differentiation, and collagen production thus resulting in thicker skin with a smoother texture.
Through interactions with nuclear chromatin in gene expression, retinoic acid helps direct the differentiation of immature skin cells (keratinocytes) into mature cells of the epidermis. For this reason, if one is deficient in vitamin A, keratin-producing cells will replace mucus-secreting cells in several body tissues, including the GI tract, trachea, eyes, and skin.
Immune Cells
Additionally, retinoic acid is believed to help regulate the processes of proliferation and differentiation of some myeloid precursor cells of the bone marrow. For example, progenitor cells differentiate into dendritic cells given adequate retinoic acid.3 The dendritic cells, go on to function in augmenting the body’s immune response.
Growth
As of now, the specific way(s) in which vitamin A affects growth remains unclear. Overall, vitamin A’s ability to regulate cell growth seems to be cell-specific, as it induces cell death, cell cycle arrest, and/or differentiation in some cells while it augments cell survival and proliferation in other cell types.
Cell-to-Cell Communication
Researchers have some ideas. For example, it’s thought that the role vitamin A plays in cell growth regulation may have something to do with gap junctions and cell-to-cell communication.
Gap junctions are cell-to-cell channels that are formed by connexin proteins. They’re needed for numerous reasons including for the exchange of small signaling compounds which allow for cell-to-cell communication.
Retinoic acid and 4-oxoretinoic acid have been shown to increase the synthesis of connexin 43, a type of gap junction protein, by stabilizing connexin 43 mRNA.4 Given that a lack of gap junction communication leads to uncontrolled cell growth (as with cancer cells), vitamin A is thought to play a big role in keeping cell growth in check.
Cell Adhesion, Recognition, and Aggregation
Retinol may contribute to cell growth through its role in glycoprotein synthesis. Retinol plus ATP generate retinyl phosphate, which can be converted to retinyl phosphomannose, which in turn can transfer mannose to glycoprotein acceptors, causing them to become mannosylated glycoproteins.
Such changes to glycoproteins can have a profound effect on tissue cell differentiation via their effects on cell recognition, adhesion, and aggregation.
Other Functions
Without going into detail, here’s a short list of other functions vitamin A is thought to play:5
- Reproduction in both males and females (mechanism unclear).
- Bone maintenance and development via its effects on osteoclasts and/or osteoblasts. Too little and too much of the vitamin can have negative effects on bone mineral density).
- Bone cell and platelet production—vitamin A seems to be involved in hematopoiesis (the production of platelets and blood cells that occurs in the bone marrow).
- Immune function—for example, retinoic acid, which is made in some immune cells, stimulates killer cell activity, phagocytosis, and cytokine production.
Carotenoids
Antioxidant Functions
Above, we briefly went over the structure of carotenoids. Well, the conjugated double bonds we talked about as being present in the side chains (often nine or more) are what make carotenoids fat-soluble. They’re also what gives the class of compounds their characteristic ability to act as antioxidants by quenching oxygen and free radicals (molecules or atoms having one or more unpaired electrons). Vitamin E plays the same roles, but functions largely in cell membranes.
Quenching of Singlet Molecular Oxygen
“Quenching” is the process wherein excited molecules/atoms are inactivated. Singlet molecular oxygen molecules, for example, are inactivated by this quenching process. Oxygen in singlet form has a higher energy state and is thus much more reactive than ground state molecular oxygen.
Carotenoids are present in lipid membranes which is convenient, given that singlet oxygen comes about by the lipid peroxidation of membranes.
Other ways in which singlet molecular oxygen is generated includes:
- The transfer of light energy (photochemical reactions)
- The respiratory/oxidative burst that occurs in some phagocytic cells
- The redox reactions of superoxides.
Anyway, however, generated, singlet molecular oxygen easily reacts with lipids, protein, and DNA in a way that damages cellular components.
Carotenoids like beta carotene and lycopene quench these trouble-making singlet oxygen molecules via their conjugated double-bond systems. Of all the carotenoids, lycopene seems to be the most effective in quenching singlet oxygen.6
Carotenoids react with the singlet oxygen, receiving its energy allowing the oxygen to return to ground state. The carotenoids’ new found energy is then released—it doesn’t need regenerating like vitamins E and C.
Quenching of Free Radicals
Beta carotene and other carotenoids also have the ability to react with free radicals—specifically, peroxyl radicals, one that causes lipid peroxidation. By quenching these molecules, carotenoids help prevent cellular and DNA damage.
When it comes to scavenging free radicals and preventing lipid peroxidation, beta-carotene seems to work synergistically with vitamin E. The latter (vitamin E) is thought to function on the membrane surface, while beta-carotene seems to function on the interior of the membrane.
This forms a carotenoid radical that are stabilized by the carotenoid’s double bonds until the molecule is ultimately decomposed. I mentioned above that lycopene seems to be the most effective in quenching singlet oxygen. Again, at least in chemical assays, lycopene has been shown to be the strongest antioxidant.6
In descending order, the in vitro antioxidant power ranking is as follows:6
- Lycopene
- Vitamin E (as α-tocopherol)
- α-carotene
- β-cryptoxanthin
- zeaxanthin
- β-carotene
- Lutein
Various combinations of the above work even better. Vitamin E and beta carotene were mentioned. Also, lycopene and lutein seem to be especially effective.
Significance
Because carotenoids are able to react with singlet oxygen and free radicals this class of compounds is thought to offer protection against several diseases.
Some epidemiological studies have shown people having high intakes of fruits and veggies, and higher serum levels of carotenoids to have a lower incidence of diseases including CVD, certain cancers, cataracts, and age-related macular degeneration. The latter two bring us to the next function.
Carotenoids and Macular Degeneration Risk (A Potential Association)
We know that carotenoids are good for eye health, at the very least, because many serve as vitamin A precursors. It so happens that carotenoids may also help prevent certain degenerative eye conditions.
Several carotenoids are found in the eyes:
- Lutein
- Zeaxanthin
- Beta carotene
Of the 20 to 30 carotenoids found in human blood and tissues, lutein and zeaxanthin are the only two found in the lens and retina.7-9
A common cause of blindness in older adults is age-related macular degeneration.
The macula, being found in the center of the retina, is responsible for central vision. It can become damaged over time. Lutein and zeaxanthin are especially concentrated in this region, and for this reason, are referred to as macular pigments. Together with beta carotene, these pigments inhibit the oxidation of cell membranes protecting the eyes from oxidative damage.
Again, most of the evidence for the protective effects of these carotenoids comes from epidemiological studies showing decreased macular degeneration risk to be associated with serum levels of carotenoids in general. While some studies have shown people with high serum concentrations of lutein and zeaxanthin to have lower risks of macular degeneration, others have failed to show an association.10-15
A few years ago the FDA concluded that no credible evidence exists to warrant health claims promoting lutein and zeaxanthin for the prevention of age-related macular degeneration.16
Carotenoids and Reduced Cataract Risk (Possible Association)
Another age-related condition of the eyes is cataracts, which affect the lens of the eye due to a buildup of abnormal proteins. The lens—which functions to focus light on the retina—can become cloudy causing vision to be impaired.
Anyway, it should come as no surprise that free radicals are thought to contribute to this process. Because zeaxanthin and lutein are found in the eye and have antioxidant capacity, they along with beta carotene are thought to potentially help prevent cataract formation.
As with macular degeneration, many studies have shown inverse associations between plasma levels of these carotenoids and cataract risk, but the results are mixed, to say the least, and the FDA position is that there’s not sufficient scientific evidence to justify recommending these specific carotenoids to lower cataract risk.16-21
However, they’re still thought to potentially help. So, consuming high amounts of plant foods high in these compounds can only improve overall health, and may or may not help prevent degenerative eye conditions.
Carotenoids and Heart Disease
A monocyte is a large phagocytic white blood cell. It runs around engulfing or gobbling up debris (oxidized molecules) for disposal.
In the events leading up to the development of atherosclerosis, cholesterol in LDLs gets oxidized and tagged for removal/disposal by the monocytes. Unfortunately, when monocytes pick up these oxidized particles for disposal, they often get lodged in artery walls where they die off and become foam cells. Foam cells become fatty streaks, and eventually progress to fibrous plaque, clogging up the arteries.
So, this process has to take place every time LDL cholesterol gets oxidized. Therefore, every time LDL cholesterol gets oxidized, of it increases the likelihood that a monocyte will bind to and be taken up by the blood vessel walls (endothelium).
It’s thought that carotenoids—including beta carotene, lutein, lycopene, and α-carotene—may prevent the oxidation of LDL cholesterol thus preventing this artery-clogging cascade from being initiated which should slow the development of atherosclerosis.
Remember, carotenoids found in whole foods are likely the most beneficial. Supplementation of beta carotene with other antioxidants in folks with coronary artery disease has been shown to effectively reduce the susceptibility of LDL to oxidation.22 However, the effectiveness of carotenoids in treating and preventing heart disease has not been established, and, for that reason, carotenoid supplementation isn’t recommended.23
Carotenoids and Cancer
Carotenoids have been shown to stimulate cell differentiation and inhibit cell proliferation while also affecting growth. For example, lycopene, both induce cell differentiation and inhibits growth and proliferation of numerous cancer cells.
In vitro, the carotenoids canthaxanthin and beta carotene have been found to inhibit neoplastic transformation (the conversion of normal cells into tumor cells) induced by carcinogens as well as inhibit the oxidation of lipids in plasma membranes.
It’s currently unknown how carotenoids actually exert these effects on cell proliferation and differentiation, but mechanisms seem to be similar to those of the retinoids covered earlier in the article. It may be that carotenoids enhance gap junction cell-to-cell communication, similar to the way retinoic acid does.
Some carotenoids have been shown to affect the gene expression of connexin 43, the protein discussed above that enables connections to be formed between cells, affecting growth and proliferation.4
Interestingly, gap Junction-style communication is inhibited in some cancer cells which may bear some relationship to the capacity of carotenoids to protect this type of communication.24
Food Over Supplements
If you read the article on skin cancer, then you know that researchers have conducted many a study on carotenoid supplementation—specifically, beta carotene—with little to show in the way of health benefits.
The CARET trial provided 30 mg of beta carotene along with 25,000 IU of vitamin A to asbestos-exposed workers and found no benefit.25
In Finland, an intervention trial provided 20 mg of beta carotene along with alpha-tocopherol (vitamin E) to long-term smokers. It was called the ATBC trial (alpha-tocopherol beta carotene). Zero benefits were found.26
As mentioned in the lung cancer article, one study found β-carotene supplementation to be associated with an increased risk of lung cancer and heart disease in these same high-risk populations (the asbestos-exposed and long-term smokers).25
Researchers aren’t necessarily in agreement about whether there is any risk in supplementing beta carotene or if the observed association was due to the presence of other cofactors. For example, it may be that the combination of beta carotene supplementation along with excessive smoking and alcohol consumption is what poses an increased risk of cancer.27,28
In any case, supplementation with beta carotene has failed to reliably show any benefits in the way of cancer prevention or anything else. The official statement from the Institute of Medicine is that “beta-carotene supplements are not advisable for the general population.”29
Recommended Daily Allowance (Needs)
As with niacin and folate, recommendations for vitamin A are expressed in vitamin equivalents. This is to account for the gap in vitamin activity between carotenoids and retinol as well as the varying vitamin activity found amongst the 50 or so carotenoids that exist. They used to be retinol equivalents (RE), but due to information that emerged a few years back, have since evolved into retinol activity equivalents (RAE).
International Units (Original System)
Early on the vitamin activity of beta carotene was thought to be about half that of retinol. Prior recommendations were based on this assumption.30,31
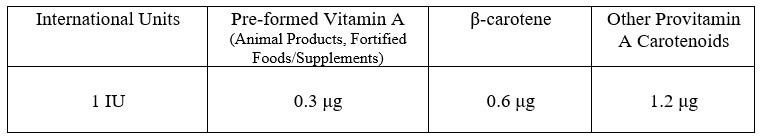
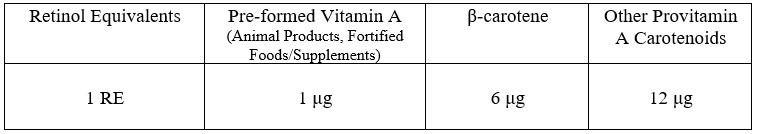
Retinol Equivalents
Then there was REs which was just another way of expressing the above numbers.

The Newer System: Retinol Activity Equivalents (RAE)
Finally, we have RAEs. From ARS (USDA), “The (new) RAE conversion factors are based on recent studies that show that the conversion of provitamin A carotenoids to retinol is only half as great as previously thought.”32
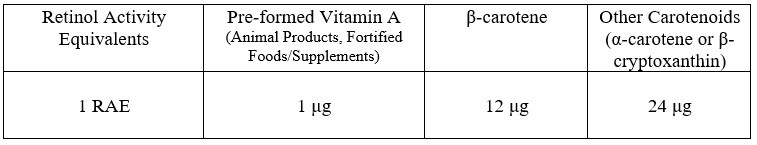
Source: adapted from Food and Nutrition Board, Institute of Medicine. Dietary Reference Intakes. Washington, DC: National Academy Press. 2001 pp. 82–161.
Basically, the previous numbers were based on pure beta carotene oil—and not beta carotene found in whole, fibrous plant foods. Dietary beta carotene turned out to have about half the vitamin activity of the pure beta carotene oil.33
Here are the updated International Unit conversions.
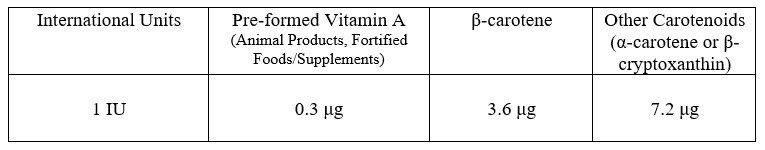
So, as you can see, you need quite a bit more beta carotene and tons more of the other carotenoids to get the same amount of vitamin activity of 1 μg of retinol. As for the implications of all of this, according to the National Institute of Medicine, “This change in bioconversion means that a larger amount of provitamin A carotenoids, and therefore darkly colored, carotene-rich fruits and vegetables, is needed to meet the vitamin A requirement.”34
The RDA for vitamin A is based on daily requirements plus this huge gap in vitamin activity.
Anyway, all this gives rise to the adult vitamin A RDAs 900 μg RAE (3,000 IU) and 700 μg RAE (2,310 IU) for men and women, respectively.34 Per usual, needs go up during pregnancy and lactation, 770 μg RAE (2,565 IU) and 1,300 μg RAE (4,300 IU), respectively.34
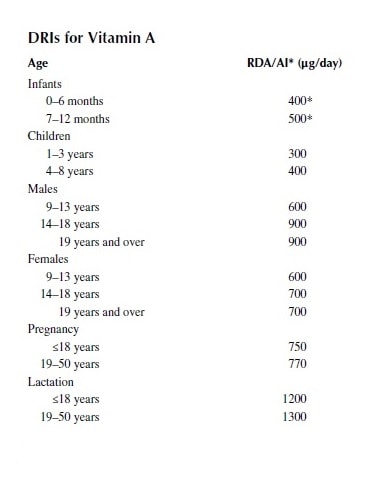
Source: Micronutrients in Health and Disease. Kedar Prasad – Crc – 2011
Values are adapted and summarized from the table of Dietary Reference Intakes (DRIs) published by www.nap.edu. RDA, Recommended Dietary Allowance; AI*, Adequate Intakes; UL, Tolerable Upper Intake Value. 1 μg retinol = 1 μg retinol activity equivalent (RAE); 1 IU (international unit) retinol = 0.3 μg retinol; and 2 μg beta-carotene = 1 μg of retinol.
Vitamin A Toxicity: Can Vegans Get Too Much?

This is a common question along with “where can I find a vegan multivitamin without vitamin A?” Can vegans get too much vitamin A?
It depends on what you mean. Can vegans get too much preformed vitamin A from supplements and/or fortified foods? Absolutely. The Tolerable Upper Intake Level (TUL) for preformed vitamin A is 3,000 μg RAE/day which comes to about 10,000 IU.34
Chronically going over the TUL for a time causes the vitamin to build up in the system leading to toxicity. Amounts upwards of 50,000 IU of vitamin A taken over a short time can result in acute hypervitaminosis A.
Symptoms of this condition include:35
- Nausea and vomiting
- Increased intracranial pressure (ICP)
- Headache
- Double or blurred vision
- Dizziness
- Skin desquamation
- Muscle incoordination
If referring to toxicity from provitamin A (naturally occurring in food), then the answer is no. All you risk is taking on a nice glow–a condition known as carotenodermia. Babies tend to get this when they eat too much carrot food. It’s a completely benign condition caused by the buildup of carotenoids in the skin.
Vegan Sources
Pre-formed Vitamin A (Fortified Plant Foods and Supplements)
Keep in mind that the main form of vitamin A in fortified foods is as retinyl esters (retinyl palmitate, etc.). So, we’re talking about pre-formed vitamin A. Unlike carotenoids, you can get too much of pre-formed vitamin A.1
As for pharmaceutical vitamin A preparations, all-trans-retinyl palmitate, and all-trans-retinyl acetate are common. There’s also a water-soluble form of vitamin A called Aquasol A, which is used for folks with fat malabsorptive disorders.
One Tbsp. of margarine typically has 500 IU (10% DV).36 One cup of raisin bran usually has 743 IU (15% DV).37
Carotenoids
Vitamin A Activity
Sure, they don’t offer the same vitamin activity of pre-formed vitamin A, but carotenoids do go a long way in helping people reach their vitamin A requirements. Approximately 26% and 34% of vitamin A activity in men and women, respectively, is from provitamin A carotenoids.33
As for which plants are best for getting provitamin A carotenoids, according to the same IOM report, “Ripe, colored fruits and cooked, yellow tubers are more efficiently converted to vitamin A than equal amounts of dark green, leafy vegetables.”34
- Bright red fruits and veggies. 1 cup of cherry tomatoes has 1241 IU (25% DV). 1 Cup of diced watermelon has 876 IU (18% DV).39,40
- Orange fruits and veggies. For example, papayas, pumpkin, and persimmons. 1 large carrot has 2068 IU (41% DV).41
- Green leafies. Don’t be fooled by the green color—the chlorophyll is the dominant pigment and masks the carotenoid content which can be significant. For example, 1 cup of kale has 10302 IU which comes to 206% of the DV.42
- Broccoli. 1 large stalk has 4334 IU (87% DV).43
As Antioxidants and Phytonutrients
For another, they seem to offer many health benefits beyond vitamin A activity. They’re antioxidants, phytonutrients, anti-cancer, you name it.
Carotenoids common to the most widely consumed plant foods include:38
- α-carotene
- β-carotene—broccoli, peas, spinach, cantaloupe, squash
- β-cryptoxanthin—fruits of all kinds
- Lutein—broccoli, kiwi, and beets
- Lycopene—tomatoes, tomato products, and watermelon.
- Zeaxanthin—orange peppers, potatoes, and corn
Select Vitamin A Sources
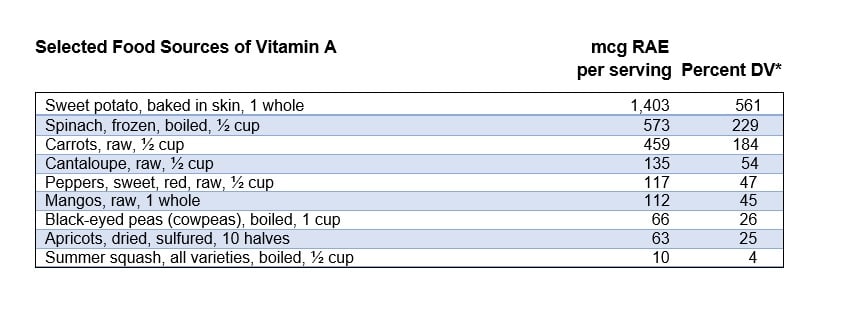
Deficiency Symptoms
Through interactions with nuclear chromatin in gene expression, retinoic acid helps direct the differentiation of immature skin cells (keratinocytes) into mature cells of the epidermis. Vitamin A deficiency has long been characterized in animals by impaired growth that can be stimulated with replacement by either retinol or retinoic acid.
While vitamin A deficiency in the US tends to be much less common compared to less developed countries, it does happen—especially for those with certain conditions:
- Malabsorptive disorders. They usually suffer from steatorrhea (or greasy stools due to excessive fecal fat content). This condition is common in those with health issues affecting the small intestine, colon, liver, pancreas, and gallbladder.
- Acute infections and intestinal parasites
- Measles—a condition thought to worsen vitamin A status by diminishing intake, and absorption, while increasing urinary excretion of vitamin A.44
- Acute protein deficiency
- Chronic nephritis
I mentioned in the opening of the article that a group at risk for vitamin A deficiency are people in developing countries, especially women and children. Kids under 5 in developing countries tend to have inadequate intake of this vitamin leading to depleted stores and frank deficiency contributing to increased mortality rates.
Several ocular (eye) effects can result from vitamin A deficiency:35
- Night blindness (often one of the first symptoms) results from impaired rhodopsin production in the rod cells of the retina.
- Xerophthalmia—marked dryness of the eyes due to inadequate mucus production. With keratinization of epithelial cells, mucus-secreting cells are replaced by keratin-producing cells in many body tissues including the eyes. Goblet cells in the conjunctiva disappear further contributing to the problem.
- Xerosis of the cornea and Bitot’s spots—keratinization of the cornea’s cells leading to corneal xerosis and Bitot’s spots. The latter (Bitot’s spots) results from sloughed off cells mixing with secretions forming a white, foamy accumulation in the eyes. If left untreated, xerosis can lead to scarring of the cornea, corneal perforations, and even blindness.
Other signs and symptoms of vitamin A deficiency include:35
- Anorexia and undernutrition in general
- Retarded growth
- Impaired immune function and increased susceptibility to infections
- Enlargement of hair follicles
- Keratinization of epithelial cells—as mentioned, mucus-secreting cells are replaced by keratin-producing cells various body tissues, including the skin, GI tract, and trachea.
The Vegan Diet and Vitamin A Status
Overall, vitamin A status isn’t a huge area of concern. According to the Institute of Medicine (US) Panel on Micronutrients’s Table 4.6 the vitamin A content of a well-planned vegan diet with carotene-rich fruits and veggies should come to about 1,262 RAE which is well within the guidelines for adult men and women.33
If you tend not to use supplements or fortified foods and rely heavily on carotenoids then try to incorporate plenty of cooked yellow tubers and ripe, colored fruits in your diet as they tend to be more efficiently converted to vitamin A compared to dark green, leafy vegetables.
References
- Gropper, Sareen S.; Smith, Jack L.. Advanced Nutrition and Human Metabolism (Page 372).
- Office Of Dietary Supplements – Vitamin A https://ods.od.nih.gov/factsheets/VitaminA-HealthProfessional/
- Hengesbach L, Hoag K. Physiological concentrations of retinoic acid favor myeloid dendritic cell development over granulocyte development in cultures of bone marrow cells in mice. J Nutr. 2004; 134:2653–59.
- Sies H, Stahl W. Carotenoids and intercellular communication via gap junctions. Int J Vit Nutr Res. 1997; 67:364–67.
- Gropper, Sareen S.; Smith, Jack L.. Advanced Nutrition and Human Metabolism (Page 384).
- Sies H, Stahl W. Vitamin E and C, β-carotene, and other carotenoids as antioxidants. Am J Clin Nutr. 1995; 62(suppl):S1315–21.
- Parker RS. Carotenoids in human blood and tissues. J Nutr. 1989;119:101–102.
- Yeum KJ, Shang F, Schalch W, Russell RM, Taylor A. Fat-soluble nutrient concentrations in different layers of human cataractous lens. Curr Eye Res. 1999;19:502–505.
- Bone RA, Landrum JT, Tarsis SL. Preliminary identification of the human macular pigment. Vision Res. 1985;25:1531–1535.
- SanGiovanni JP, Chew EY, Clemons TE, et al. The relationship of dietary carotenoid and vitamin A, E, and C intake with age-related macular degeneration in a case-control study: AREDS Report #22. Arch Ophthalmol. 2007; 125:1225–32.
- Moeller SM, Parekh N, Tinker L, et al. Associations between intermediate age-related macular degeneration and lutein and zeaxanthin in the Carotenoids in Age-Related Eye Disease Study (CAREDS): Ancillary Study of the Women’s Health Initiative. Arch Ophthalmol. 2006; 124:1151–62.
- Flood V, Smith W, Wang JJ, et al. Dietary antioxidant intake and incidence of age-related maculopathy: the Blue Mountain Eye Study. Ophthalmology. 2002; 109:2272–78.
- Cho E, Seddon JM, Rosner B, et al. Prospective study of intake of fruits, vegetables, vitamins and carotenoids and risk of age-related maculopathy. Arch Ophthalmol. 2004; 122:883–92.
- Parisi V, Tedeschi M, Gallinaro G, et al. Carotenoids and antioxidants in age-related maculopathy Italian study: multifocal electroretinogram modifications after 1 year. Ophthalmology. 2008; 115:324–33.
- Age-related Eye Disease Study Research Group: A randomized placebo-controlled clinical trial of high dose supplementation with vitamins C and E, β carotene, and zinc for age-related macular degeneration and vision loss. Arch Ophthalmol. 2001; 119:1417–36.
- Trumbo PR, Ellwood KC. Lutein and zeaxanthin intakes and risk of age-related macular degeneration and cataracts: an evaluation using the Food and Drug Administration’s evidence-based review system for health claims. Am J Clin Nutr. 2006; 84:971–74.
- Christen WG, Liu S, Glynn RJ, et al. Dietary carotenoids, vitamins C and E, and risk of cataract in women: a prospective study. Arch Ophthalmol. 2008; 126:102–09.
- Fernandez MM, Afshari NA. Nutrition and the prevention of cataracts. Curr Opin Ophthalmol. 2008; 19:66–70.
- Chiu C, Taylor A. Nutritional antioxidants and age-related cataract and maculopathy. Exp Eye Res. 2007; 84:229–45.
- Tan AG, Mitchell P, Flood VM, et al. Antioxidant nutrient intake and the long-term incidence of age-related cataract: the Blue Mountains Eye Study. Am J Clin Nutr. 2008; 87:1899–1905.
- Chylack LT, Brown NP, Bron A, et al. The Roche European American Cataract Trial (REACT): a randomized clinical trial to investigate the efficacy of an oral antioxidant micronutrient mixture to slow progression of age-related cataract. Ophthalmic Epid. 2002; 9:49–80.
- Mosca L, Rubenfire M, Mandel C, et al. Antioxidant nutrient supplementation reduces the susceptibility of low-density lipoprotein to oxidation in patients with coronary artery disease. J Am Coll Cardiol. 1997; 30:392–99.
- Voutilainen S, Nurmi T, Mursu J, Rissanen T. Carotenoids and cardiovascular health. Am J Clin Nutr. 2006; 83:1265–71.
- Acevedo P, Bertram J. Liarozole potentiates the cancer chemopreventive activity of and the up-regulation of gap junctional communication and connexin 43 expression by retinoic acid and β-carotene in 10T1/2 cells. Carcinogenesis. 1995; 16:2215–22.
- Omenn G, Goodman G, Thomquist M, et al. Effects of a combination of β carotene and vitamin A on lung cancer and cardiovascular disease. N Engl J Med. 1996; 334:1150–55.
- α-tocopherol, β-carotene (ATBC) Cancer Prevention Study Group: the effect of vitamin E and β carotene on the incidence of lung cancer and other cancers in male smokers. N Engl J Med. 1994; 330:1029–35.
- Omenn G, Goodman G, Thornquist M, et al. Risk factors for lung cancer and for intervention effects in CARET, the β-carotene and retinol efficacy trial. J Natl Cancer Inst. 1996; 88:1550–59.
- Mayne S, Handelman G, Beecher G. β-carotene and lung cancer promotion in heavy smokers: a plausible relationship? J Natl Cancer Inst. 1996; 88:1513–15.
- Food and Nutrition Board, Institute of Medicine. Dietary Reference Intakes. Washington, DC: National Academy Press. 2000 pp. 325–82.
- NRC (National Research Council). 1980. Recommended Dietary Allowances, 9th ed. Washington, DC: National Academy Press.
- NRC. 1989. Recommended Dietary Allowances, 10th ed. Washington, DC: National Academy Press.
- Composition of Foods Raw, Processed, Prepared USDA National Nutrient Database for Standard Reference, Release 20 USDA, Feb. 2008. https://www.ars.usda.gov/ARSUserFiles/80400525/Data/SR20/SR20_doc.pdf
- Read “Dietary Reference Intakes For Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc” At Nap.edu https://www.nap.edu/read/10026/chapter/6#120
- Food and Nutrition Board, Institute of Medicine. Dietary Reference Intakes. Washington, DC: National Academy Press. 2001 pp. 82–161.
- Gropper, Sareen S.; Smith, Jack L.. Advanced Nutrition and Human Metabolism (Page 388).
- Margarine, Margarine-type Vegetable Oil Spread, 70% Fat, Soybean and Partially Hydrogenated Soybean, Stick Nutrition Facts & Calories https://nutritiondata.self.com/facts/fats-and-oils/636/2
- Cereals Ready-to-eat, Malt-o-meal, Raisin Bran Cereal Nutrition Facts & Calories https://nutritiondata.self.com/facts/breakfast-cereals/9145/2
- Gropper, Sareen S.; Smith, Jack L.. Advanced Nutrition and Human Metabolism (Page 373).
- Tomatoes, Red, Ripe, Raw, Year Round Average [includes Usda Commodity Food A238, A233] Nutrition Facts & Calories https://nutritiondata.self.com/facts/vegetables-and-vegetable-products/2682/2
- Watermelon, Raw Nutrition Facts & Calories https://nutritiondata.self.com/facts/fruits-and-fruit-juices/2072/2
- Carrots, Baby, Raw Nutrition Facts & Calories https://nutritiondata.self.com/facts/vegetables-and-vegetable-products/3026/2
- Kale, Raw Nutrition Facts & Calories https://nutritiondata.self.com/facts/vegetables-and-vegetable-products/2461/2
- Broccoli, Cooked, Boiled, Drained, Without Salt Nutrition Facts & Calories https://nutritiondata.self.com/facts/vegetables-and-vegetable-products/2357/2
- Stephensen C. Vitamin A, infection, and immune function. Ann Rev Nutr. 2001; 21:167–92.
- Jose L. Revuelta, Ruben M. Buey, Rodrigo Ledesma‐Amaro, and Erick J. Microbial biotechnology for the synthesis of (pro)vitamins, biopigments and antioxidants: challenges and opportunities. Microb Biotechnol. 2016 Sep; 9(5): 564–567.
- Animal-derived Ingredients Resource | Living https://www.peta.org/living/food/animal-ingredients-list/

